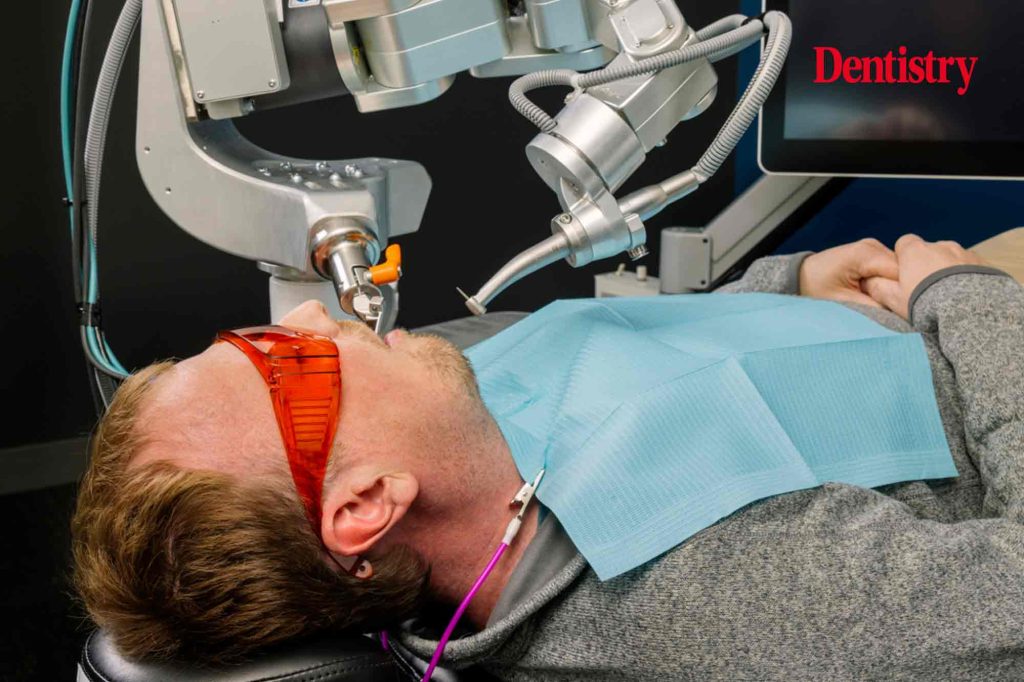
Robotic-assisted systems are revolutionizing nearly every aspect of modern medicine, and dentistry is no exception. Oral surgery—long known for its need for precision, stability, and clinician expertise—is undergoing a remarkable transformation as robotics enter the dental operatory. While still emerging, robotic technologies are rapidly improving surgical accuracy, reducing complications, enhancing training, and reshaping what patients can expect from complex procedures.
In this in-depth exploration, we look at how robotics is changing the game in oral surgery, focusing on three major areas: precision cutting, recovery benefits, and the evolving training requirements for clinicians using these systems.
Why Are Robotics Becoming Central to Oral Surgery?
Oral surgery demands a high level of technical skill. Even slight hand tremors or misalignments can impact nerves, bone structures, or implant positioning. Robotics offer a solution by providing assistance, stabilization, and computer-guided precision that humans alone cannot achieve consistently.
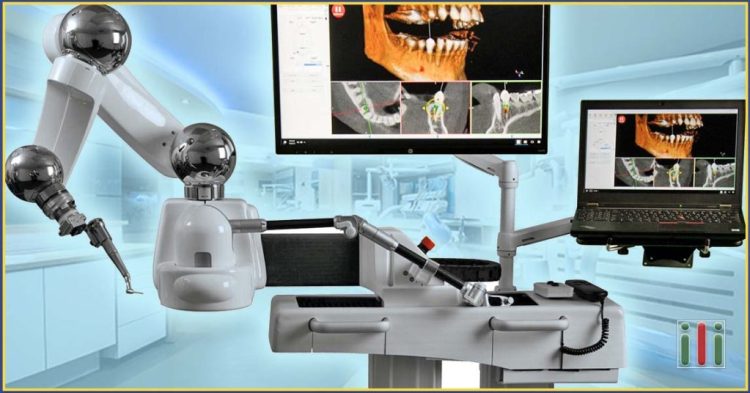
Robotic systems used in dentistry—such as Yomi for implant placement—combine real-time imaging, haptic feedback, and mechanical guidance, enabling surgeons to work with better control and predictability. These tools not only support surgeons but also elevate the standard of care delivered to patients.
How Do Robots Improve Precision Cutting in Oral Surgery?
1. Accuracy Beyond Human Limitations
Robotic systems are designed to enhance precision by:
- Guiding drill angles using preoperative scans
- Ensuring depth control to avoid nerve damage
- Sub-millimeter accuracy in implant placement
This level of precision is challenging to achieve manually, especially in challenging anatomical conditions such as narrow ridges, dense bone, or proximity to delicate structures.
2. Real-Time Imaging Integration
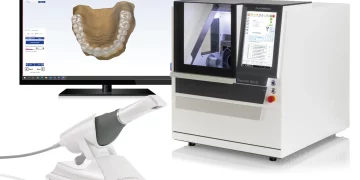
Robots can integrate CBCT scans, intraoral scans, and digital planning files to create a surgical map. During the procedure:
- The system continuously monitors the drill position
- Deviations are corrected through haptic resistance
- The surgeon maintains control while benefiting from robotic guidance
This combination of human oversight and robotic accuracy results in highly predictable surgical outcomes.
3. Minimizing Surgical Errors
Precision cutting reduces the chance of:
- Misaligned implants
- Excessive bone removal
- Accidental perforations
- Inadvertent soft-tissue trauma
By minimizing these risks, robotics is setting a new benchmark for surgical quality.
Do Robotics Reduce Recovery Time for Oral Surgery Patients?
1. Smaller Incisions and Less Tissue Trauma
Robotics allow for more conservative procedures by:
- Reducing unnecessary bone or tissue removal
- Targeting only the required surgical area
- Avoiding exploratory cuts through enhanced visualization
Smaller disruptions to tissue often translate into faster recovery and fewer postoperative complications.
2. Lower Inflammatory Responses
Precise movements minimize mechanical trauma, which can reduce:
- Swelling
- Pain
- Bruising
- Bleeding
Many patients report smoother healing experiences after robot-assisted implant placement or extraction procedures.
3. Enhanced Stability During Surgery
Robotic arms are steady, preventing micro-errors that could cause additional tissue strain. As a result:
- Suturing becomes easier
- Postoperative discomfort decreases
- Recovery timelines shorten
4. Fewer Follow-Up Complications
Because precision minimizes surgical surprises, issues such as infections, misaligned implants, or bone fractures are less frequent. This reduces the need for corrective surgeries and accelerates long-term healing.
What Training Do Surgeons Need to Use Robotics Safely and Effectively?
Robotics bring new capabilities, but they also require a significant shift in clinical training.
1. Mastering Digital Planning Systems
Surgeons must learn to:
- Interpret CBCT and digital models
- Create accurate surgical plans
- Simulate implant angles and depths
- Understand anatomical risk zones
This places more emphasis on virtual planning skills.
2. Hands-On Robotic System Training
Manufacturers typically require:
- Multi-day certification courses
- Simulation exercises
- Supervised clinical cases
Surgeons must understand both the mechanical and software components of robotic systems.
3. Integrating Robotics Into Workflow
Training involves mastering:
- Patient positioning for robotic access
- Calibrating robotic arms
- Monitoring haptic feedback
- Overriding or adjusting system controls when needed
This integration may initially lengthen procedure times until proficiency increases.
4. Understanding Limitations and Safety Protocols
Robotics are tools—not replacements for clinician expertise. Surgeons must know when to:
- Override robotic guidance
- Revert to manual instrumentation
- Adapt to unexpected anatomical findings
Experienced clinical judgment remains essential to safe outcomes.
What Are the Main Advantages of Robotics for Clinics and Practitioners?
1. Increased Predictability and Standardization
Robotics reduce variability between cases and improve consistency across clinicians.
2. Competitive Differentiation
Clinics offering robotic-assisted surgery may attract patients seeking the latest technology and highest precision.
3. Enhanced Documentation
Robotic systems record:
- Angles
- Depths
- Pathways
- Procedural metrics
This helps with quality assurance, legal protection, and patient education.
4. Reduced Physical Fatigue for Surgeons
Robotics handle much of the stabilizing work, allowing practitioners to maintain better posture and avoid ergonomic strain.
Are There Any Limitations or Drawbacks?
1. High Initial Investment
Robotic systems can cost hundreds of thousands of dollars, making them less accessible for small clinics.
2. Learning Curve
Clinicians may initially experience:
- Longer procedure times
- Increased planning requirements
- Adaptation challenges
3. Procedural Restrictions
Not all oral surgeries currently benefit from robotics. Most advancements focus on:
- Implants
- Bone grafting
- Precision drilling procedures
Complex soft-tissue surgeries are still performed manually.
4. Dependence on Digital Imaging Accuracy
Poor-quality scans can compromise robotic guidance, emphasizing the need for high-end imaging equipment.
How Will Robotics Shape the Future of Oral Surgery?
Robotics represent a major shift in surgical philosophy: from manual dexterity to digital precision and guided control. Looking ahead, we can expect:
1. Fully Autonomous Surgical Steps
Robots may one day handle repetitive drilling or measurement tasks with minimal human intervention.
2. Integration With AI Diagnostics
AI models will help predict risk areas, anatomical variations, and ideal implant trajectories—feeding directly into robotic systems.
3. More Personalized Surgeries
Patient-specific 3D models and real-time adjustments will allow robotics to tailor procedures to individual anatomy.
4. Expansion Into New Procedures
Future robotic systems may support:
- Orthognathic surgeries
- Complex extractions
- Microvascular repairs
- Endodontic microsurgery
Robotics will likely become as common in dental operating rooms as digital imaging is today.
Conclusion: Is Robotics Truly Changing the Game in Oral Surgery?
Absolutely—robotics is not just enhancing oral surgery; it is redefining it. By providing unparalleled precision, improving patient outcomes, and elevating the capabilities of clinicians, robotic-assisted surgery represents a major milestone in dental innovation.
While cost and training remain challenges, the ongoing evolution of robotic technology suggests that its adoption will continue to grow. For patients, this means safer procedures, less discomfort, and faster recovery. For clinicians, it means increased accuracy, confidence, and the ability to deliver the next generation of surgical care.
Robotics is not replacing surgeons—it is empowering them to perform at their best.



























Discussion about this post