In the ever-evolving landscape of modern dentistry, patients facing a significantly damaged tooth are presented with more options than ever before. From advanced bonding techniques to onlays and inlays, it’s natural to wonder if the traditional dental crown—a solution that has been used for over a century—is still the best choice. Is it an outdated, overly aggressive treatment, or does it remain the undisputed champion for saving compromised teeth? The answer is nuanced. While newer, more conservative options are excellent for certain situations, the dental crown continues to hold a critical and irreplaceable role in restorative dentistry. Its enduring value lies in its unique ability to provide comprehensive protection, unparalleled strength, and long-term predictability for teeth that are beyond the help of a simple filling. This article will delve deep into the world of dental crowns, exploring the specific problems they solve, the modern materials available, the intricate process of getting one, and how to ensure it lasts for decades, providing a clear-eyed view of why this classic treatment is far from obsolete.
1. The Unmatched Protector: Key Indications for a Dental Crown
A dental crown, often called a “cap,” is a custom-made restoration that encases the entire visible portion of a tooth, restoring its shape, size, strength, and appearance. It is not a first-line treatment for minor decay but a strategic solution for specific, serious dental problems.
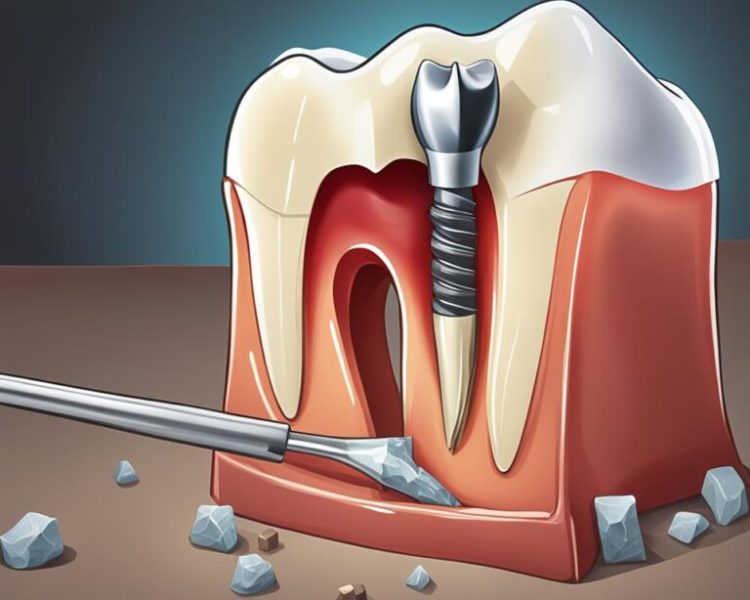
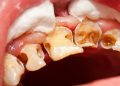
Structural Compromise: This is the most common reason for a crown. When a tooth has a large fracture or has lost a significant portion of its structure to decay or a large old filling, it becomes weak and prone to splitting under chewing forces. A crown encircles the tooth, holding it together like a barrel held together with metal hoops, preventing a catastrophic fracture that would necessitate an extraction.
Post-Root Canal Therapy: A root canal procedure removes the infected pulp from inside the tooth, but in doing so, it hollows out the tooth, making it dry and brittle. Without the protective crown, a root-canaled tooth is highly susceptible to fracture. A crown is not just recommended after a root canal; it is essential for the long-term survival of the tooth.
Severe Wear and Tear: Teeth can be worn down over time due to bruxism (grinding), acid erosion (from diet or GERD), or attrition. When the enamel is severely diminished, the teeth become sensitive, functionally compromised, and aesthetically unappealing. Crowns can rebuild the teeth to their proper dimensions, protecting them from further damage and restoring a functional bite.
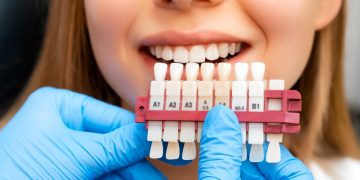
Cosmetic Enhancement: For teeth that are severely discolored, misshapen, or misaligned and cannot be improved with simpler options like veneers or whitening, crowns offer a complete aesthetic transformation. They can create a perfectly shaped, sized, and colored tooth, making them a cornerstone of full-mouth rehabilitation and smile makeovers.
Abutment for a Dental Bridge: When a tooth is missing, a fixed bridge uses the teeth on either side of the gap as supports. These abutment teeth must be crowned to securely hold the prosthetic tooth (pontic) in place.

2. The Material World: Navigating Modern Crown Choices
The “one-size-fits-all” metal crown of the past is gone. Today, the choice of material is a careful balance between strength, aesthetics, location in the mouth, and cost.
All-Ceramic or All-Porcelain: These crowns provide the best natural color match and translucency, making them the most aesthetically pleasing option. They are highly biocompatible and an excellent choice for people with metal allergies.
- Zirconia: A super-strong, durable ceramic that is virtually unbreakable. Modern zirconia can be layered with porcelain to achieve excellent aesthetics, making it suitable for both front and back teeth. It is the material of choice for strength and reliability.
- Lithium Disilicate (e.g., E-max): Renowned for its exceptional balance of strength and lifelike beauty. It is incredibly translucent and strong enough for most crowns, particularly on front teeth and premolars.
Porcelain-Fused-to-Metal (PFM): This was the workhorse of cosmetic dentistry for decades. It features a metal substructure for strength, covered with a layer of tooth-colored porcelain. PFMs are very strong and durable. The main drawback is the opaque metal core, which can create a darker line at the gumline over time, especially if the gums recede. They are a reliable and cost-effective option for back teeth.
Gold Alloys: The classic standard for durability and biocompatibility. Gold crowns are extremely strong, wear down at a rate similar to natural enamel (making them gentle on opposing teeth), and require the least amount of healthy tooth structure to be removed. Their primary disadvantage is their conspicuous metallic color, limiting their use to less visible back teeth for most patients.
Base Metal Alloys: Made from non-noble metals like nickel or chromium, these crowns are highly resistant to corrosion and very strong. They also require minimal tooth preparation. However, the potential for nickel allergies and their dark silver appearance makes them a less popular choice today.
3. The Journey to a New Crown: The Detailed Preparation Steps
Getting a crown is a meticulous, multi-step process typically completed over two appointments, ensuring precision and a perfect fit.
First Appointment: Preparation and Impression
- Diagnosis and Treatment Planning: The dentist examines the tooth, takes X-rays, and discusses the material options with the patient.
- Anesthesia: The tooth and surrounding gum are completely numbed for a comfortable experience.
- Tooth Reshaping: Using a dental drill, the dentist carefully removes a uniform layer of enamel from all surfaces and the top of the tooth. The amount removed depends on the material chosen (metal crowns require less removal than all-ceramic ones).
- Impression: Once the tooth is perfectly shaped, a highly accurate digital scan or a traditional physical impression is taken of the prepared tooth and the opposing teeth. This is sent to a dental laboratory where a skilled technician will fabricate the permanent crown, a process that usually takes about two weeks.
- Temporary Crown: A temporary acrylic crown is cemented over the prepared tooth. This temporary protects the tooth, maintains the space, and allows for normal eating and appearance while the permanent crown is being made.
Second Appointment: Placement
- Temporary Removal: The temporary crown is carefully removed, and the tooth is cleaned.
- Fit and Bite Check: The permanent crown is tried in. The dentist checks the fit against the gumline, the contact with adjacent teeth, and the bite (occlusion), making any necessary adjustments.
- Cementation: Once the fit is perfect, the tooth is isolated and dried. The crown is then permanently cemented onto the prepared tooth using a strong dental adhesive.
4. Investing in Longevity: What is the Real Lifespan of a Crown?
A dental crown is a significant investment, and understanding its lifespan is crucial. On average, a well-made and well-cared-for crown can last between 10 and 15 years. However, it is not uncommon for crowns to last 25-30 years or even a lifetime with exceptional oral hygiene and regular dental care.
The lifespan is influenced by several key factors:
- Oral Hygiene: The leading cause of crown failure is not the crown breaking, but decay forming at the margin where the crown meets the tooth. This area is vulnerable and must be kept clean.
- Personal Habits: Habits like teeth grinding (bruxism), chewing ice, biting fingernails, or using teeth as tools can dramatically shorten a crown’s life.
- Material Selection: Zirconia and gold crowns are renowned for their exceptional durability, while all-porcelain crowns may be more prone to chipping over time, though modern materials have greatly improved.
- The Skill of the Dentist and Lab Technician: A precise fit is paramount. A poorly fitting crown will trap plaque and lead to premature failure.
5. Preserving Your Investment: Essential Care and Maintenance Tips
Caring for a crowned tooth is similar to caring for a natural tooth, but with a few added points of attention.
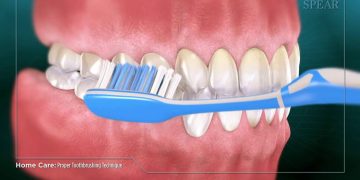
Meticulous Oral Hygiene: Brush twice a day with a non-abrasive toothpaste and floss daily. It is especially important to floss carefully at the gumline around the crown to disrupt the plaque biofilm that leads to decay and gum disease.
Regular Professional Cleanings: Visit your dentist every six months (or as recommended) for a check-up and cleaning. Your dentist will use professional tools to clean around the crown and check for any signs of wear, chipping, or decay at the margins.
Wear a Night Guard: If you grind or clench your teeth at night, a custom-fitted night guard from your dentist is non-negotiable. It will protect both your natural teeth and your crown investment from excessive forces that can cause fractures or wear.
Avoid Destructive Habits: Be mindful of your crown. Do not chew on hard objects like ice, popcorn kernels, or pens. Try to avoid sticky candies that could potentially dislodge the crown over time.
So, are dental crowns still the best option? For teeth that are broken, root-canaled, or structurally compromised, the answer is a resounding yes. No other restorative treatment offers the same level of comprehensive protection and predictable, long-term success. While less invasive options should always be considered first for smaller problems, the dental crown remains the gold standard for saving severely damaged teeth. It is a time-tested, technologically advanced solution that, when indicated and cared for properly, can reliably preserve your natural tooth for a lifetime.



























Discussion about this post