You look at it every day when you brush your teeth, but how often do you actually see it? Your tongue is more than just an organ for taste and speech; it is a mirror reflecting the intricate workings of your entire body. Often overlooked in self-health assessments, the tongue can provide early, crucial clues to systemic illnesses, nutritional deficits, and localized infections that might otherwise go unnoticed. Its color, texture, coating, and overall appearance are a dynamic map of your well-being. This article will serve as your guide to interpreting this map, empowering you to understand what’s normal and, more importantly, recognizing the signs that warrant a deeper investigation into your health.
1. The Landscape of Health: Decoding Colors and Textures
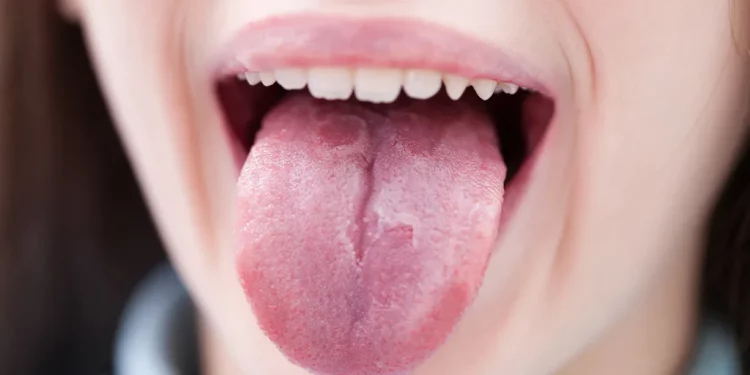
A healthy tongue is typically pink, moist, and covered with tiny, pinkish-white nodules called papillae, which give it a uniformly slightly rough texture. Any significant deviation from this baseline can be significant.
Color Changes: A Chromatic Warning System
- Bright Red (Strawberry or Raspberry Tongue): A tongue that turns a vibrant, beefy red can be a sign of several conditions. It is a classic symptom of Kawasaki disease, a rare but serious illness in children that causes inflammation in blood vessels. In adults, it can indicate a deficiency of Vitamin B12 or folic acid, as these nutrients are essential for maintaining the papillae. When they are lacking, the tongue can become smooth and inflamed, a condition known as glossitis. Scarlet fever, a streptococcal infection, also presents with a “strawberry tongue” early on.
- White Coating or Patches: A thin, white coating is often harmless and can be related to mild dehydration or debris. However, thick, white, curd-like patches that can be scraped off may indicate a oral thrush, a yeast infection caused by Candida albicans. If the white patches are lacy, web-like, or cannot be scraped away (a condition called leukoplakia), it could be a reaction to an irritant, like tobacco, or in some cases, a precancerous change.
- Black and Hairy Tongue: This alarming but usually harmless condition occurs when the papillae on the tongue grow long and trap dead skin cells, bacteria, and debris. The discoloration—which can also be brown, green, or yellow—comes from bacterial pigments and staining from food or tobacco. It is often linked to poor oral hygiene, antibiotic use, dry mouth, or excessive coffee/tea consumption.
- Yellow Coating: A yellow tongue is typically a precursor to black hairy tongue, caused by the same buildup of bacteria and debris. It can also be a sign of gastric reflux or, less commonly, liver or gallbladder issues.
- Pale Tongue: A pale, whitish-pink tongue can simply be a sign of being cold. However, if it is consistently pale and accompanied by fatigue, it could point to iron-deficiency anemia, where a lack of red blood cells reduces the tongue’s healthy red color.
Texture and Surface Changes: Feeling the Difference
- Geographic Tongue (Benign Migratory Glossitis): This harmless, inflammatory condition causes map-like, red, smooth patches to appear on the surface of the tongue, often with slightly raised, white borders. These patches “migrate,” healing in one area and appearing in another, sometimes over a period of days. The cause is unknown, and it typically requires no treatment.
- Fissured Tongue (Scrotal Tongue): Characterized by deep grooves or fissures on the dorsal surface, this is often a genetic, harmless trait. However, these grooves can trap food and bacteria, increasing the risk of infection or bad breath if the tongue is not cleaned thoroughly.
- Burning Tongue Syndrome: This condition involves a burning sensation on the tongue without any visible clinical signs. It can be linked to nutritional deficiencies, dry mouth, hormonal changes, nerve damage, or psychological factors.

2. The Infection Alert: Recognizing Signs of Illness
Your tongue is often the first place where signs of a systemic or localized infection become visible.
Oral Thrush (Candidiasis): As mentioned, this appears as creamy white, raised lesions on the tongue and inner cheeks. They may bleed slightly when scraped. While common in infants, it can occur in adults with weakened immune systems, uncontrolled diabetes, or those using steroid inhalers or antibiotics.
Scarlet Fever: Caused by the same bacteria as strep throat, this infection produces a toxin that causes a characteristic “white strawberry tongue” (white coating with red dots) that later peels to reveal a “red strawberry tongue.”
Oral Herpes and Hand, Foot, and Mouth Disease (HFMD): Both of these viral infections can cause small, painful blisters or ulcers to form on the tongue and elsewhere in the mouth. HFMD is common in young children and is accompanied by a rash on the hands and feet.
Syphilis: In its primary stage, a syphilis infection can cause a single, painless sore (chancre) on the tongue. In its secondary stage, it can produce white patches or mucous patches.
Hairy Leukoplakia: Unlike the potentially precancerous leukoplakia, this version is caused by the Epstein-Barr virus and is almost exclusively seen in people with severely compromised immune systems, such as those with HIV/AIDS. It appears as white, hairy or corrugated patches on the sides of the tongue that cannot be scraped off.
3. The Silent Signal: Your Tongue and Nutrient Deficiencies
The state of your tongue is exquisitely sensitive to your nutritional status. Chronic deficiencies can manifest in clear, though not always specific, ways.
The B-Vitamin Complex: Deficiencies in B vitamins, particularly B12, B6, folate (B9), and riboflavin (B2), are classic culprits behind tongue changes. The deficiency causes the papillae to atrophy, leading to a condition called atrophic glossitis. The tongue becomes smooth, shiny, inflamed, and beefy red, and is often painful. This is commonly seen in pernicious anemia (an inability to absorb B12) and in those with poor diets.
Iron Deficiency Anemia: Iron is crucial for producing hemoglobin, which gives blood its red color. A lack of iron not only pales the tongue but can also lead to inflammation and soreness (glossitis), making it appear smooth and swollen.
Niacin (Vitamin B3) Deficiency (Pellagra): A severe niacin deficiency, though rare in developed countries, causes the tongue to become bright red, swollen, and painful. It is part of a syndrome characterized by the “three Ds”: dermatitis, diarrhea, and dementia.
Zinc Deficiency: A lack of zinc can impair taste perception (dysgeusia) and can contribute to the development of fissures on the tongue and delayed wound healing in the mouth.
4. The Foundation of a Healthy Tongue: The Critical Role of Hygiene
Many tongue abnormalities are directly linked to oral hygiene practices—or the lack thereof. The tongue’s rough surface is the primary reservoir for the bacteria that cause bad breath (halitosis) and contribute to plaque formation on teeth.
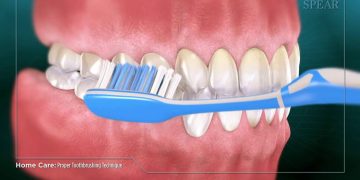
Tongue Cleaning: A toothbrush alone is not enough. Using a dedicated tongue scraper is the most effective way to remove the layer of bacteria, dead cells, and food debris that coats the tongue. A gentle scraping from the back to the front, repeated several times, can significantly improve oral freshness and reduce the bacterial load in the entire mouth.
The Link to Overall Oral Health: A dirty tongue contributes directly to the formation of plaque on teeth, increasing the risk of cavities and gum disease (gingivitis and periodontitis). Maintaining a clean tongue is a non-negotiable part of a complete oral care routine.
Debunking Myths: Contrary to some beliefs, vigorous scraping or brushing will not damage a healthy tongue’s papillae. The key is to be gentle but thorough. Furthermore, mouthwash is not a substitute for mechanical cleaning; it should be used as an adjunct to, not a replacement for, scraping or brushing.
5. Navigating the Signs: When to See a Doctor or Dentist
While many tongue changes are temporary and harmless, certain signs are red flags that demand professional evaluation.
Persistent Changes: Any change in the color or texture of your tongue that lasts for more than two weeks should be examined by a dentist or doctor. This is the most important rule of thumb.
Lumps, Sores, or Ulcers: A lump on the tongue, a sore that doesn’t heal, or a persistent ulcer must be taken seriously. These are the primary warning signs for oral cancer, especially if they are painless initially.
Pain or Burning: Unexplained pain, soreness, or a persistent burning sensation that interferes with eating or speaking warrants an investigation to rule out deficiencies, infections, or neurological issues.
Difficulty Moving or Swallowing: Any loss of mobility, swelling that restricts movement, or difficulty swallowing is a significant sign that requires immediate medical attention.
Combined Symptoms: Pay attention if tongue changes are accompanied by other symptoms like a high fever, skin rashes, unexplained weight loss, or fatigue. This combination often points to a systemic issue that needs a comprehensive diagnosis.
Your tongue is a powerful, accessible diagnostic tool. By taking a moment to observe it each day, you can become an active participant in your health journey. A bright pink, clean tongue is a welcome sign of well-being. But a black, white, red, or painfully smooth tongue is your body’s way of sending an S.O.S. signal. Learning to interpret these signals—and knowing when to seek professional help—can make all the difference in catching minor issues before they become major problems and in maintaining not just oral health, but your overall vitality.



























Discussion about this post