Diabetes and gum disease share a powerful, two-way connection that many people don’t realize until symptoms have already become severe. High blood sugar doesn’t only affect your heart, eyes, nerves, and kidneys—it also deeply influences your oral health. In fact, people with diabetes are significantly more likely to develop gum disease, and untreated gum infection can make diabetes harder to control.
Understanding this cycle early is the key to protecting both your smile and your overall well-being.
Below, we explore in depth how diabetes affects gum tissues, how inflammation spreads, the signs you should watch for, and what steps can stop the progression.
1. How Does Diabetes Affect the Gums?
Diabetes influences gum health through multiple biological pathways. Most of the damage stems from elevated blood glucose and impaired immune response.
Reduced Blood Flow to the Gums
Diabetes thickens blood vessel walls, decreasing circulation throughout the body—including the gums. Poor blood flow means fewer nutrients and less oxygen reach the gum tissues, making them more susceptible to infection and slower to heal after irritation.
Weakened Immune System
High blood sugar interferes with the body’s ability to fight harmful bacteria. As plaque and calculus accumulate on teeth, diabetic patients have a harder time combating the resulting inflammation. This gives harmful bacteria the upper hand, allowing gum disease to progress faster and more aggressively.
Higher Glucose Levels in Saliva
When blood sugar is elevated, saliva also contains more glucose. Bacteria thrive in sugar-rich environments, creating ideal conditions for gum infections to take hold.
Dry Mouth (Xerostomia)
Diabetes is often associated with reduced saliva production. Since saliva helps wash away food particles and neutralize acids, a dry mouth increases the risk of plaque buildup, irritation, and gum inflammation.
Slow Healing of Gum Tissue
Even minor gum injuries, such as those caused by brushing or flossing improperly, can take longer to heal in people with diabetes. This makes the gums more vulnerable to chronic infections.
Together, these factors make diabetic individuals far more prone to gingivitis and periodontitis—often at younger ages and with more severe outcomes.
2. How Does the Inflammation Cycle Develop in Diabetics?
The relationship between diabetes and gum disease is often described as a vicious cycle, in which one condition intensifies the other.
Step 1: High Blood Sugar Fuels Bacterial Growth
Excessive glucose encourages harmful bacteria in the mouth to multiply. These bacteria produce toxins that irritate the gums and start the inflammatory process.
Step 2: Inflammation Harms Gum Tissues
Inflamed gums pull away from the teeth, forming pockets that trap more bacteria and debris. This deepens the infection, further fueling inflammation.
Step 3: Inflammation Disrupts Blood Sugar Control
Chronic gum inflammation increases the body’s overall inflammatory load, releasing cytokines that make insulin less effective. As a result, blood sugar becomes harder to manage.
Step 4: High Blood Sugar Causes Further Gum Damage
Poorly controlled diabetes accelerates gum deterioration, bone loss, and pocket formation. This loops back into worsening inflammation.
The Cycle Continues
Without intervention, this back-and-forth impact leads to severe gum disease, tooth mobility, tooth loss, and elevated diabetes complications.
Breaking this cycle requires managing both gum infection and blood sugar simultaneously—a coordinated medical and dental effort.
3. What Symptoms Should Diabetic Patients Watch For?
Because gum disease can move faster in diabetic individuals, early detection is essential. Take these symptoms seriously—even mild ones may indicate a developing issue.
Common Early Signs
- Red, swollen, or tender gums
- Bleeding when brushing or flossing
- Persistent bad breath
- Dry mouth or thick, stringy saliva
- Gum discomfort that comes and goes
Moderate to Severe Symptoms
- Receding gums exposing more tooth root
- Pus between the teeth and gums
- Pain when chewing
- Teeth feeling loose or shifting
- Formation of deep gum pockets
Systemic Clues
Diabetic patients may notice:
- Worsening blood sugar control
- Slower healing of mouth sores
- More frequent oral infections
If any symptoms persist longer than a few days, a dental evaluation is necessary. Early treatment can prevent extensive damage.

4. How Can Diabetics Prevent Gum Disease?
Prevention is far more effective and less costly than treatment—especially for people living with diabetes.
Maintain Stable Blood Sugar Levels
Good glycemic control is the most important factor. Studies show that patients who maintain healthy A1C levels develop fewer gum problems and respond better to treatment.
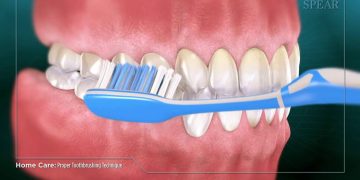
Establish an Effective Oral Hygiene Routine
- Brush twice daily with a soft toothbrush and fluoride paste.
- Floss once a day to remove debris between teeth.
- Consider using an antibacterial or alcohol-free mouthwash.
- Replace your toothbrush every 2–3 months.
Keep a Regular Dental Checkup Schedule
Diabetic patients should visit the dentist at least twice a year, sometimes more frequently if early signs of gum disease are present.
Manage Dry Mouth
- Sip water regularly.
- Use sugar-free lozenges or xylitol gum.
- Ask your dentist or doctor about saliva substitutes if needed.
Eat a Balanced Diet
Choosing foods that control blood glucose while minimizing oral acidity helps protect gums and teeth.
Quit Smoking if Applicable
Smoking multiplies gum disease risk and makes diabetes harder to control. Quitting provides immediate benefits to gum health.
5. What Treatment Options Are Available for Gum Disease in Diabetic Patients?
Treatment must address infection, inflammation, and systemic health simultaneously.
Professional Cleaning and Scaling
Deep cleaning (scaling and root planing) removes plaque and tartar below the gumline. This is usually the first line of defense and often leads to significant improvements.
Antibacterial Therapy
Depending on severity, dentists may use:
- Antimicrobial rinses
- Localized antibiotic gels
- Oral antibiotics in advanced cases
These treatments help reduce bacterial load and restore gum tissue health.
Laser Therapy
Some dental clinics offer laser-assisted gum therapy, which can reduce pocket depth and bacterial levels with minimal discomfort.
Surgical Treatment for Severe Cases
If gum disease has advanced significantly:
- Flap surgery to clean deep pockets
- Bone grafts or tissue regeneration
- Soft tissue grafts to restore receded gums
Surgeries are more successful when diabetes is well managed.
Coordinated Medical Care
Dentists may collaborate with endocrinologists to ensure blood sugar control improves alongside gum treatment.
Post-Treatment Maintenance
Diabetic patients often require more frequent cleanings—as often as every 3–4 months—to keep inflammation controlled.
Conclusion: Why Understanding This Connection Matters
The relationship between diabetes and gum disease is not optional or minor—it is biologically intertwined. Elevated blood sugar weakens gum tissues, and gum infection in turn worsens blood sugar control. Recognizing this connection empowers people with diabetes to take proactive steps to break the cycle.
With consistent oral hygiene, stable blood glucose, and timely dental care, it’s entirely possible to protect your gum health and safeguard your long-term wellness.



























Discussion about this post